Trigeminal neuralgia is a chronic neurological condition characterised by sudden, severe facial pain often described as an electric shock or stabbing sensation. It affects the trigeminal nerve, which carries sensory signals from the face to the brain and controls muscles involved in chewing.
Pain episodes may occur repeatedly throughout the day and can be triggered by routine activities such as speaking, eating, brushing teeth or lightly touching the face. Although symptoms may begin as brief and infrequent episodes, trigeminal neuralgia often progresses over time, becoming more intense, longer-lasting and disruptive to daily life.
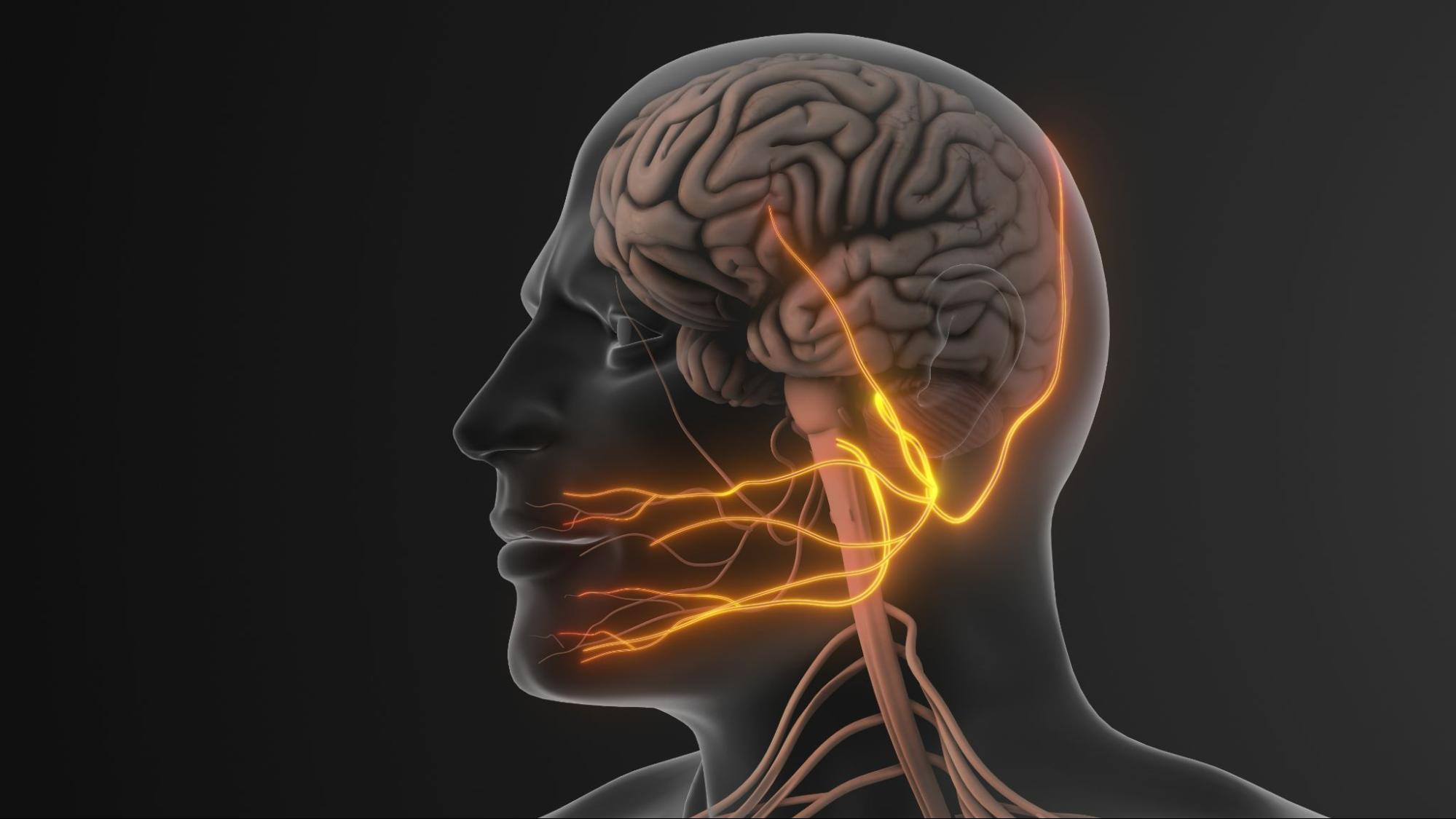
The trigeminal nerve is the fifth cranial nerve and the largest sensory nerve of the face. It branches into three divisions:
These branches provide sensation to the face and control mastication. Trigeminal neuralgia occurs when this nerve becomes irritated, most commonly at its root entry into the brainstem.

The condition develops when the trigeminal nerve becomes irritated or damaged, disrupting the normal transmission of sensory signals from the face to the brain. This irritation causes the nerve to misfire, resulting in sudden, intense pain episodes even in response to light stimulation.
Some of the common causes are:
Facial pain can arise from a wide range of conditions and not all facial pain is caused by nerve disorders. Trigeminal neuralgia is distinct because it produces sudden, severe, electric shock-like pain that is often triggered by light touch or simple facial movements.
Condition | Typical Pain Characteristics | Common Triggers | Key Distinguishing Features |
Trigeminal neuralgia | Sudden, sharp, electric shock-like pain | Touching the face, chewing, speaking, brushing teeth | Brief but intense episodes, usually one-sided, triggered by light stimulation |
Dental pain | Constant or throbbing ache | Biting, chewing, hot or cold foods | Localised to a tooth or gum, often linked to decay or infection |
Sinusitis | Dull pressure or fullness in the face | Bending forward, nasal congestion | Often accompanied by nasal symptoms, headache or fever |
TMJ disorder | Aching jaw or facial pain | Jaw movement, clenching or grinding teeth | Jaw clicking, stiffness or limited mouth opening |
The symptoms typically affect one side of the face. It may also involve one or more branches of the trigeminal nerve, which include:
Although trigeminal neuralgia can affect anyone, certain factors increase the likelihood of developing the condition by making the trigeminal nerve more vulnerable to irritation or compression.

An accurate diagnosis, by doctors experienced in neurological and facial pain conditions, is essential to confirm trigeminal neuralgia and to identify any underlying cause that may require targeted treatment. Because facial pain can arise from many conditions, careful evaluation helps ensure appropriate management.
The diagnosis involves:

Treatment aims to relieve pain, reduce nerve irritation and restore quality of life. Management is individualised based on symptom severity, underlying cause and response to previous treatments. Many patients experience meaningful improvement with non-surgical options, while others may benefit from interventional or surgical care.
It may include:
Trigeminal neuralgia is a chronic neurological condition that causes sudden, severe facial pain and can significantly disrupt daily activities such as eating, speaking and personal care. Although the condition is not life-threatening, its impact on comfort, function and emotional well-being can be substantial if left untreated.
The good news is that effective treatment options are available. With accurate diagnosis and a personalised treatment approach, many individuals experience meaningful pain relief and improved quality of life. Early assessment allows symptoms to be managed before they become more severe or persistent.
If facial pain has been affecting your daily life, seeking medical advice early can make a significant difference in long-term comfort and control.
Trigeminal neuralgia itself is not life-threatening. However, it can be caused by serious underlying conditions such as tumours or aneurysms. Proper evaluation is important to identify the cause and guide appropriate treatment.
The condition usually affects one side of the face. Bilateral symptoms are uncommon and may suggest an underlying neurological condition such as multiple sclerosis.
Pain may be triggered by everyday activities such as talking, chewing, brushing teeth, shaving or touching the face. Stress, fatigue and smoking can also increase pain frequency or intensity.
Trigeminal neuralgia is unlikely to resolve permanently without treatment. While symptoms may temporarily subside, pain episodes typically recur and often become more frequent or severe over time. Early medical assessment helps prevent worsening symptoms.
Not necessarily. Treatment depends on the underlying cause and how well symptoms respond to therapy. Some individuals achieve long-term relief and can reduce or stop medication, while others may require ongoing management to maintain comfort.
In many individuals, pain episodes become more frequent, severe or prolonged over time. Delayed treatment can significantly affect daily function, nutrition and emotional well-being.
No. Many patients experience good pain control with medication or minimally invasive treatments. Surgery is typically reserved for severe cases that do not respond to conservative management.
You should seek medical attention if facial pain is frequent, persistent or described as sharp or electric shock-like. Although symptoms may come and go, trigeminal neuralgia is a chronic condition that rarely resolves on its own. Early treatment can significantly improve symptom control.
Seek urgent medical attention if facial pain is accompanied by any of the following symptoms, as they may indicate a more serious neurological condition rather than typical trigeminal neuralgia:
These symptoms require prompt evaluation to rule out conditions such as stroke, tumour or significant nerve damage.
Dr Wilson Tay is skilled in ultrasound-guided pain interventions that provide safer, more precise relief without unnecessary radiation exposure. His expertise covers a wide range of conditions including spine pain, headaches, abdominal and pelvic pain, fibromyalgia and cancer pain.


MMed (Anaes) | FIPP (World Institute of Pain, USA) | FAMS (Anaes) | Grad Dip Acupuncture (Singapore)
Consultant Pain Specialist, Consultant Anaesthesiologist, Registered Acupuncturist MBBS
Dr Wilson Tay is skilled in ultrasound-guided pain interventions that provide safer, more precise relief without unnecessary radiation exposure. His expertise covers a wide range of conditions including spine pain, headaches, abdominal and pelvic pain, fibromyalgia and cancer pain.