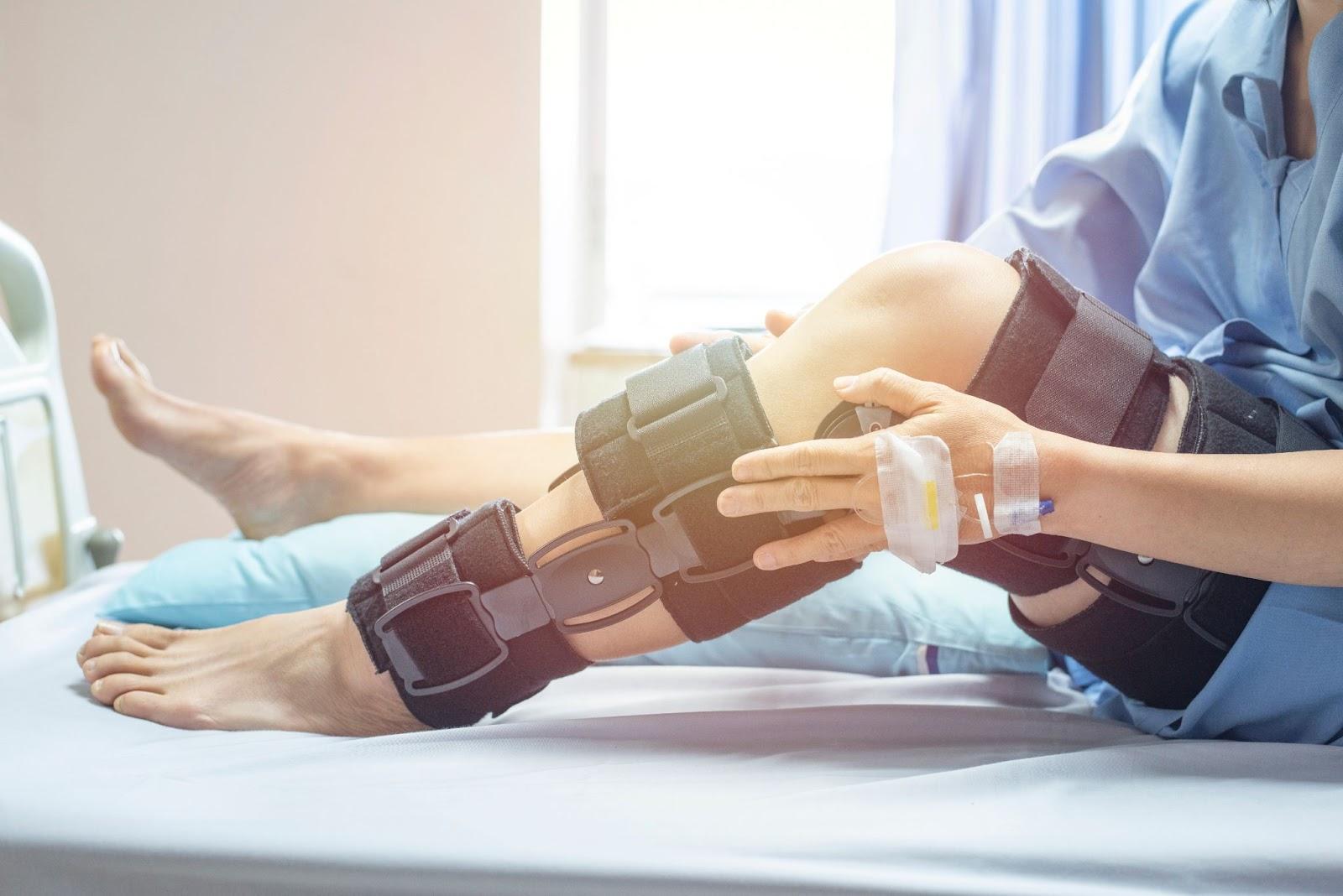
Post-surgical pain refers to the pain experienced after a surgical procedure. It is the body’s natural response to tissue injury and typically occurs as part of the healing process. Depending on the type of surgery, this pain can vary in location, intensity, and duration, ranging from mild discomfort to more severe and persistent symptoms.
The nature of post-surgical pain is influenced by several factors. These include the surgical site, the extent of tissue trauma, whether nerves were affected during the operation, the individual’s overall health, pain threshold and previous pain experiences. For most patients, this pain is temporary and improves steadily in the days or weeks following surgery. However, in some cases, it may persist for longer than expected, developing into a condition known as chronic post-surgical pain.
Post-surgical pain can present in several different forms, depending on the type of procedure, the areas involved, and individual factors such as age, underlying health conditions, and previous pain experiences.
While post-surgical pain is commonly categorised based on duration — acute, subacute, and chronic — other types such as neuropathic and referred pain may also occur, particularly when nerves are involved or pain radiates beyond the site of surgery. Each type has distinct characteristics and implications for recovery.
Post-surgical pain arises from a combination of physical, neurological, and inflammatory responses triggered by surgical intervention. While pain is a normal and expected part of recovery, its intensity and duration can vary widely depending on several contributing factors.
Patients who are anxious before surgery or have a history of depression may report higher pain levels, as emotional states influence how the brain interprets pain signals.
In most cases, post-surgical pain is a temporary and manageable part of recovery. However, when multiple factors interact, such as significant tissue trauma combined with nerve involvement or delayed healing, the pain may become more complex and require specialised management.
Post-surgical pain can present in different ways depending on the type of surgery, area affected, and the individual’s overall health. Recognising common symptoms can help identify whether the pain is following a typical recovery course or requires further attention.
If post-surgical pain does not gradually improve or starts to worsen over time, it is important to seek medical review to rule out complications or the development of chronic pain.
While post-surgical pain is common, some individuals are more likely to experience severe, prolonged, or chronic pain after surgery. Various patient-related and procedure-related factors can increase this risk.

While some level of pain is expected after surgery, there are several ways to minimise its intensity, reduce the risk of complications, and prevent it from becoming persistent or chronic. Prevention begins before the surgery itself and continues throughout the recovery period.
A post-surgical pain assessment is a structured process used to evaluate the nature, severity, and impact of a patient’s pain following surgery. It helps guide treatment decisions and ensures that pain management strategies are working effectively.
A thorough pain assessment is a key part of post-operative care. It not only improves patient comfort but also helps prevent complications and supports a smoother recovery.
Treating post-surgical pain effectively is essential to support recovery, improve mobility, and prevent complications such as chronic pain. Management typically involves a tailored, multimodal approach — combining medications, regional anaesthesia techniques, and non-drug therapies to target different pain pathways.
The goal of treatment is not to eliminate all pain, but to reduce it to a manageable level that allows rest, movement, and healing. Pain management plans are adjusted over time based on how the patient is responding and whether symptoms are resolving as expected.
Post-surgical pain arises as a natural response to tissue injury during surgery and can vary in intensity, duration, and presentation. While most patients experience acute pain that improves with healing, some may develop prolonged or nerve-related pain that requires closer attention. Factors such as the type of surgery, existing health conditions and emotional well-being can influence the severity and persistence of pain.
If you are scheduled for surgery or experiencing ongoing discomfort after a procedure, schedule a consultation with us for tailored pain relief and comprehensive post-operative care.
Yes, it’s common to feel pain in areas such as the neck, shoulders, or back due to factors like positioning during surgery or referred pain.
It’s advisable to take pain medication as prescribed, even during the night, to maintain consistent pain control and prevent discomfort from escalating.
Non-drug approaches such as applying cold or heat packs, engaging in gentle movement, practicing relaxation techniques, and using TENS units can complement pain management strategies.
Proper pain control can accelerate recovery, reduce the risk of complications like pneumonia or blood clots, and improve overall comfort and mobility.
Any changes to medication should be discussed with your healthcare provider to ensure safety and effectiveness.
A sudden increase in pain could indicate a complication. It’s important to contact your healthcare provider promptly for assessment.
Pain duration varies depending on the type of surgery and individual factors, but acute pain typically subsides within a few days to weeks.
Some over-the-counter medications may interact with prescribed drugs. Always consult your healthcare provider before combining medications.
PCA allows patients to self-administer predetermined doses of pain medication through a programmable pump, which provides control over pain relief within safe limits.
Yes, factors like anxiety, stress, and previous pain experiences can affect how pain is perceived and managed. Addressing these can improve pain control.
Dr Wilson Tay is skilled in ultrasound-guided pain interventions that provide safer, more precise relief without unnecessary radiation exposure. His expertise covers a wide range of conditions including spine pain, headaches, abdominal and pelvic pain, fibromyalgia and cancer pain.


MMed (Anaes) | FIPP (World Institute of Pain, USA) | FAMS (Anaes) | Grad Dip Acupuncture (Singapore)
Consultant Pain Specialist, Consultant Anaesthesiologist, Registered Acupuncturist MBBS
Dr Wilson Tay is skilled in ultrasound-guided pain interventions that provide safer, more precise relief without unnecessary radiation exposure. His expertise covers a wide range of conditions including spine pain, headaches, abdominal and pelvic pain, fibromyalgia and cancer pain.